Centre for Healthy Ageing
Understanding what drives cellular ageing.

About the centre
At the Centre for Healthy Ageing, we’re focused on understanding what drives cellular ageing and how this biological process causes disease. We use this information to treat and aid the prevention of diseases of ageing including dementia, liver failure and sarcopenia/frailty to promote health ageing.
We’re developing innovative nanoparticle drug delivery systems to prevent chronic liver disease, new therapeutics to repair damaged blood vessels in the brain for Alzheimer’s disease and exploring novel treatments to prevent muscle wasting during hospitalisation.
Centre Head
Laboratories
The laboratories operating within this centre are:
-
Gamble
Understanding the ageing process of the cells that make up the blood vessels, particularly in the brain, and the impact of these changes in Alzheimer’s disease, cerebral amyloid angiopathy and other cardiovascular disease. -
Philp
Understanding the factors that cause age-associated muscle weakness to develop therapeutics to prevent sarcopenia. -
Seth
Exploring the mechanisms of liver injury and identify potential biomarkers for prevention, diagnosis and therapy.
Student opportunities
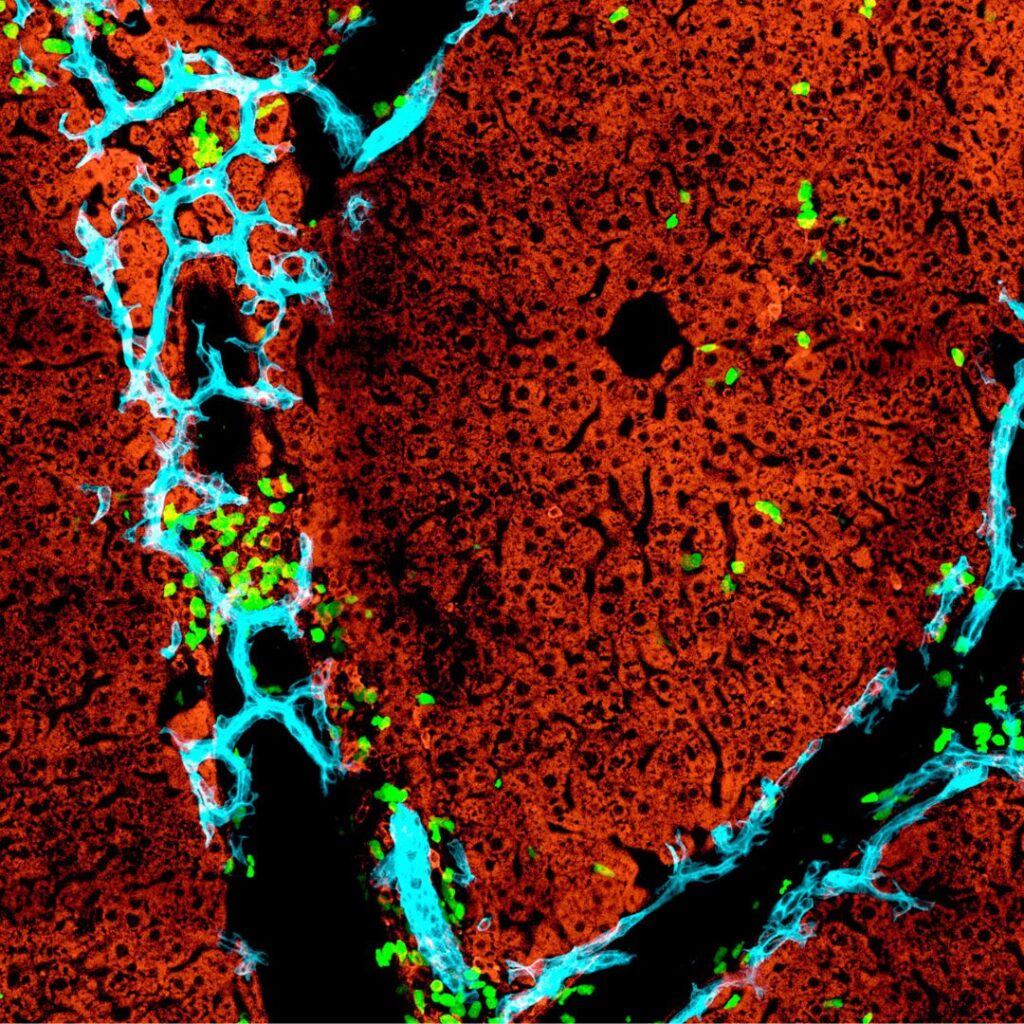
Applying genetic risk algorithm to identify patients at high risk of chronic liver diseases
Projects: PhD
Project details
Primary Supervisor: Clinical Professor Devanshi Seth
Supervisory Team: Clinical Professor Devanshi Seth
Centre: Healthy Ageing
Liver cirrhosis is one of the most common life-threatening diseases. Alcohol misuse is the major cause of alcohol-related cirrhosis (ALC), followed by the metabolic dysfunction-associated steatotic liver disease (MASLD), affecting a quarter of global adults. ALC contributes to approximately half of all liver disease related mortality with a median survival post-hospital admission of 2.5 years, worse than that of many cancers. Both ALD and MASLD are preventable if detected early. But patients remain asymptomatic until advanced disease presentation, making it difficult for clinicians to predict who are at a greater risk of preventable cirrhosis and its complications, causing loss of productivity, illness, health care utilisation and death.
Genetic susceptibility to liver diseases is recent knowledge with evidence of shared genetic risks between ALC and MASLD. Our genomic studies in ALC recently developed genetic algorithms combining clinical risk (diabetes) that can predict a 10-fold increased cirrhosis risk in drinkers (PMC8803006) and a polygenic risk score (PRSALC) that also identifies high-risk MASLD patients (PMC11093576). This new knowledge allows us to identify people at the highest risk of progressive liver damage. However, genetic testing for liver diseases is not currently practiced leaving a gap in early identification and treatment of high-risk patients.
With my team of multidisciplinary clinicians, geneticist and genetic statisticians we aim to (i) investigate the prevalence of cirrhosis risk alleles in diverse populations using publicly available genetic databases (UK Biobank, Medical Genome Reference Bank) and (ii) test our algorithms for risk prediction as a follow-up in our existing GenomALC and UK Biobank cohorts of drinkers. Knowing the genetic risk prevalence in diverse populations and predictability of risk algorithms has high potential of developing and evaluating the best individualised value-add treatment for the two most prevalent liver diseases.
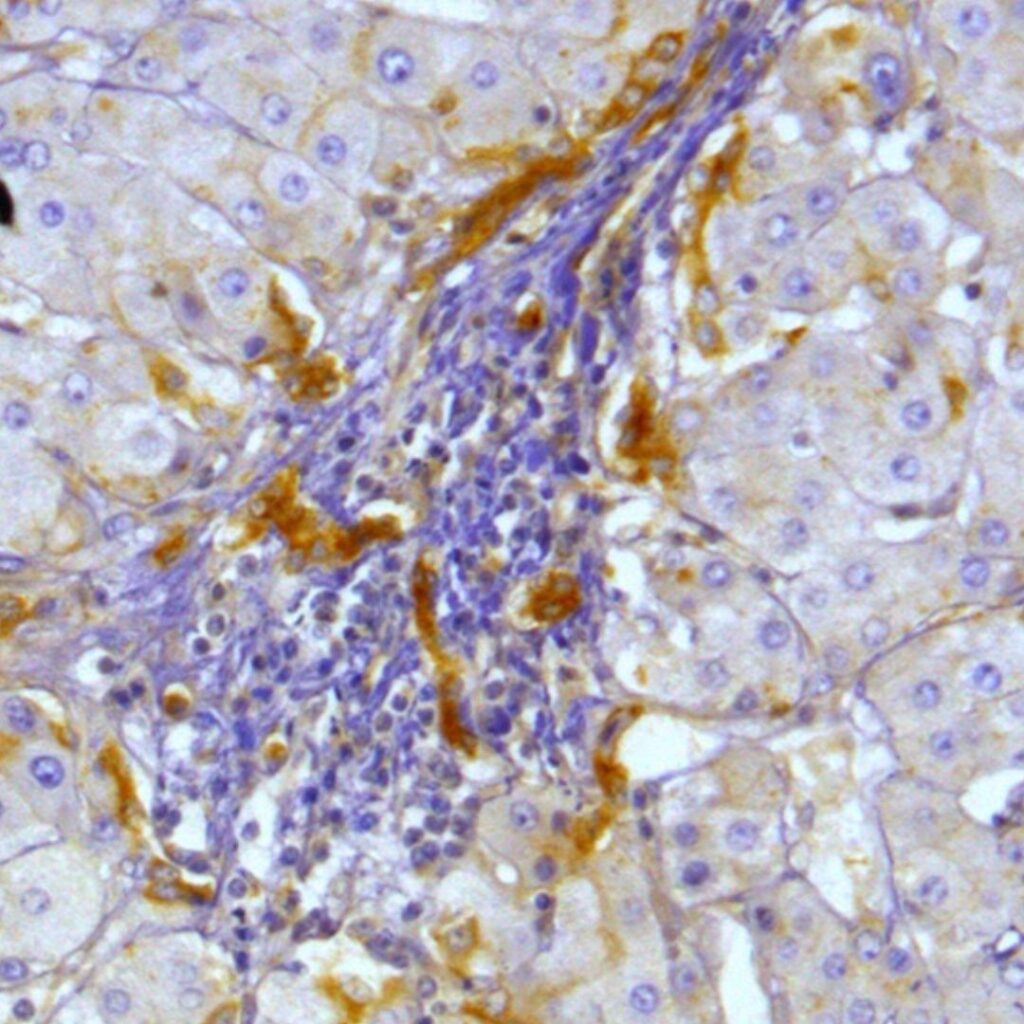
A novel nanoparticle platform targeting hepatic lipotoxicity to attenuate fatty liver diseases
Projects: PhD
Project details
Primary Supervisor: Clinical Professor Devanshi Seth
Supervisory Team: Professor Marcela Bilek, Dr Bobby Boumelhem
Centre: Healthy Ageing
Build-up of liver lipid is the first hallmark of initiation of chronic liver diseases. There is compelling evidence that fatty liver, with persistent lipid excess induces lipotoxicity, a major risk for fibrosis, cirrhosis and cancer (PMC6888337). Current pharmacological treatments focused on targeting established liver diseases remain abysmal, limited by high costs and side effects. Fatty liver diseases are reaching epidemic proportions globally, current therapies are unlikely to benefit at population level underscoring an unmet need to invest in novel directions for preventive and cost-effective therapies. New knowledge from genome wide association studies (GWAS) show that most alleles associated with risk of cirrhosis reside in genes with functions in lipid droplet biology and/or lipid metabolism, strongly linking genetic susceptibility to lipotoxicity (PMID: 32853455, PMC8803006). Thus our novel strategies proposed in this project are to (i) develop dietary nutrients (such as L-carnitine, caffeine, paraxanthine, naringenin) as therapeutic agents targeting downstream dysregulated lipid pathways associated with risk variants, and (ii) develop Plasma Polymerised Nanoparticles (PPNs) as unique drug delivery platforms to target the root cause, i.e. excess lipid driven hepatic lipotoxicity. Our team collaborators have novel IP protected ‘histochemions’, PPNs linked to Nile Red (NR) a lipophilic dye that binds to neutral lipids such as triglycerides and cholesterol, that preferentially steer histochemions towards enriched TG and cholesterol, and Nile Blue (NB) that binds to fatty acids. We have preliminary data that these histochemions can simultaneously bind to multiple cargoes covalently, including dietary nutrients and hepatocyte homing molecules (albumin, indocyanin green, asialoglycoprotein receptor), allowing specific drugs to be linked for targeting lipids and lipid pathways in the liver. This project will advance these findings, optimise delivery and intervention protocols and test the functionality of modified PPN-based drug delivery platforms in vitro (cell culture) and in vivo in our customised pre-clinical CRISPR-Cas9 risk gene depletion models of fatty liver in zebrafish (PMID37650211). Use of nutrients are already in the disease management guidelines adjunct to other therapies, as early-stage therapeutic agents. The proposed dietary nutrients are known to reduce hepatic lipotoxic injury (inflammation, mitochondrial and oxidative stress) with zero-minimal toxicity, and are the choice of drugs in this project. Our multidisciplinary team expertise in nanotechnology, genetics, biomedical engineering, lipidomics, liver diseases and clinical hepatology, preliminary data, IP protected nanoparticle platform, pre-clinical models, established protocols, core facilities (zebrafish husbandry, flow cytometry, confocal imaging) and conducive work environment, we are best placed for the successful completion of this project. This project is highly likely to generate new IP/patents and has the potential to open up avenues for exploring cost-effective therapies targeting early stages of fatty liver to prevent disease progression. Techniques: Nanotechnology, lipidomics, zebrafish husbandry, flow cytometry, confocal imaging, molecular biology, CRISPR-Cas9. Funding is being sourced through grant applications in review/to be submitted.
Get in touch
To get in touch and for all general enquiries relating to our work, please contact Professor Andy Philp.




