Centre for Cancer Innovations
Enhancing treatment outcomes for cancer patients.

About the centre
At the Centre Cancer Innovations, we’re focused on enhancing the quality of life for cancer patients. We employ innovative approaches to decipher the complex genetic and cellular mechanisms underlying various cancer types, from melanoma to liver cancer.
Our goal is to advance the development of highly effective, precisely targeted treatments.
Centre Head
Laboratories
The laboratories operating within this centre are:
-
Hogg
Investigating how proteins work in health and disease. -
Gorrell
Understanding the roles of a key enzyme family in progressive liver damage and cancer. -
Lyons
Identifying new ways of preventing and treating cancers. -
McCaughan
Understanding liver diseases and liver cancer at the cellular and molecular level. -
Tiffen
Understanding how epigenetic modifiers can drive cancer and identifying new gene targets for potential treatments. -
Yeo
Developing new treatments for patients with solid cancer tumours.
Student opportunities
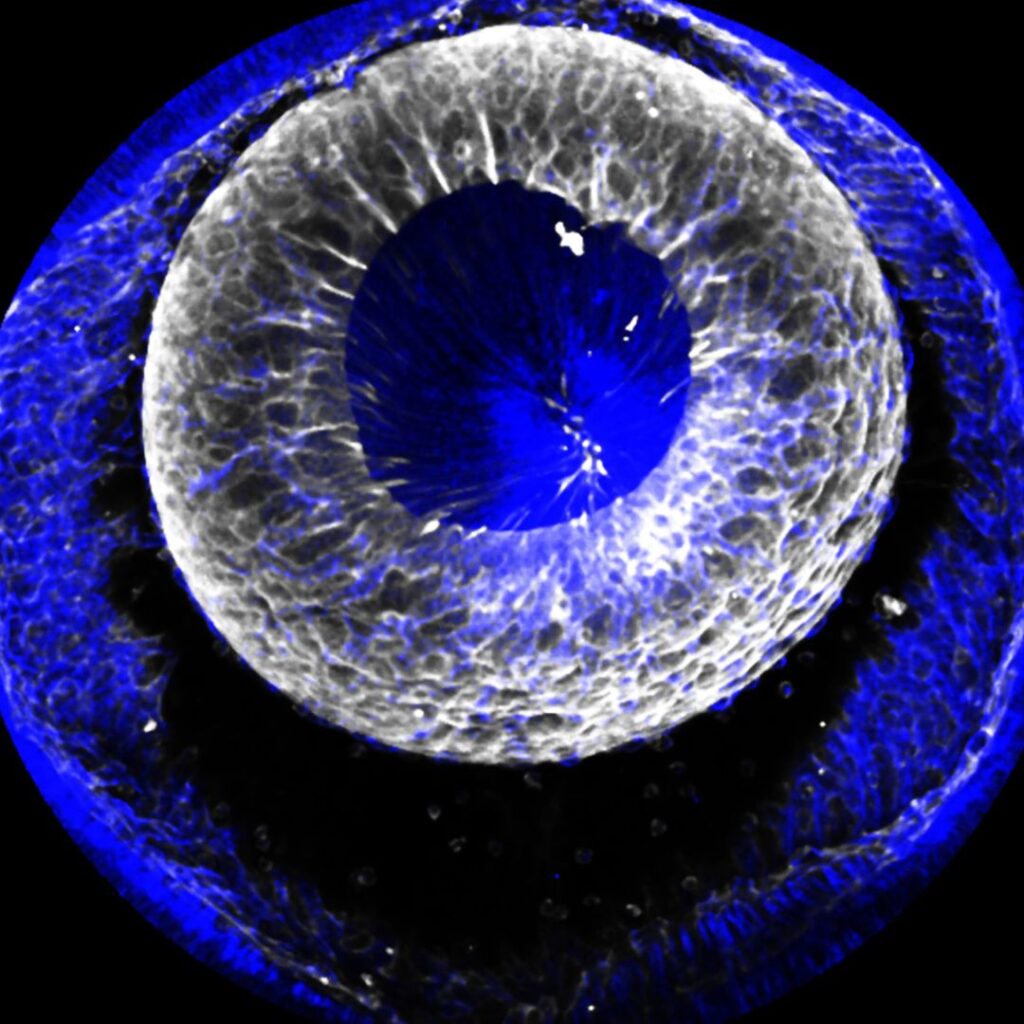
Treatment of corneal blindness using stem cells
Projects: Honours or PhD
Project details
Primary Supervisor: Associate Professor Guy Lyons
Supervisory Team: Guy Lyons, Seaky Lim, Mojdeh Abbasi
Centre: Cancer Innovations
Blindness from corneal disease affects 10 million people globally. The outermost layer of cells that cover the cornea are critical to its clarity and are produced by stem cells at its edge, called limbal stem (LS) cells. LS cell deficiency can be caused by trauma, infection or faulty genes, and is a major cause of blindness. We have developed a method for transplanting LS cells onto affected eyes via special contact lenses. However, the source remains problematic: obtaining LS cells from the other eye carries risk for that eye, and donor LS cells are often suffer immune rejection. The derivation of LS cells from patient-derived induced pluripotent stem (iPS) cells could overcome these problems. iPS cells are obtained by “re-programming” blood cells into a state that can give rise to multiple cell types. As a proof of principle of our approach, we have recently shown that iPS cells can be converted into LS cells by treating them with a special cocktail of drugs and proteins. To translate this method to the clinic, we now need to increase the efficiency of this process and enable it to occur on our special contact lenses, so that they can be transplanted safely and with ease.
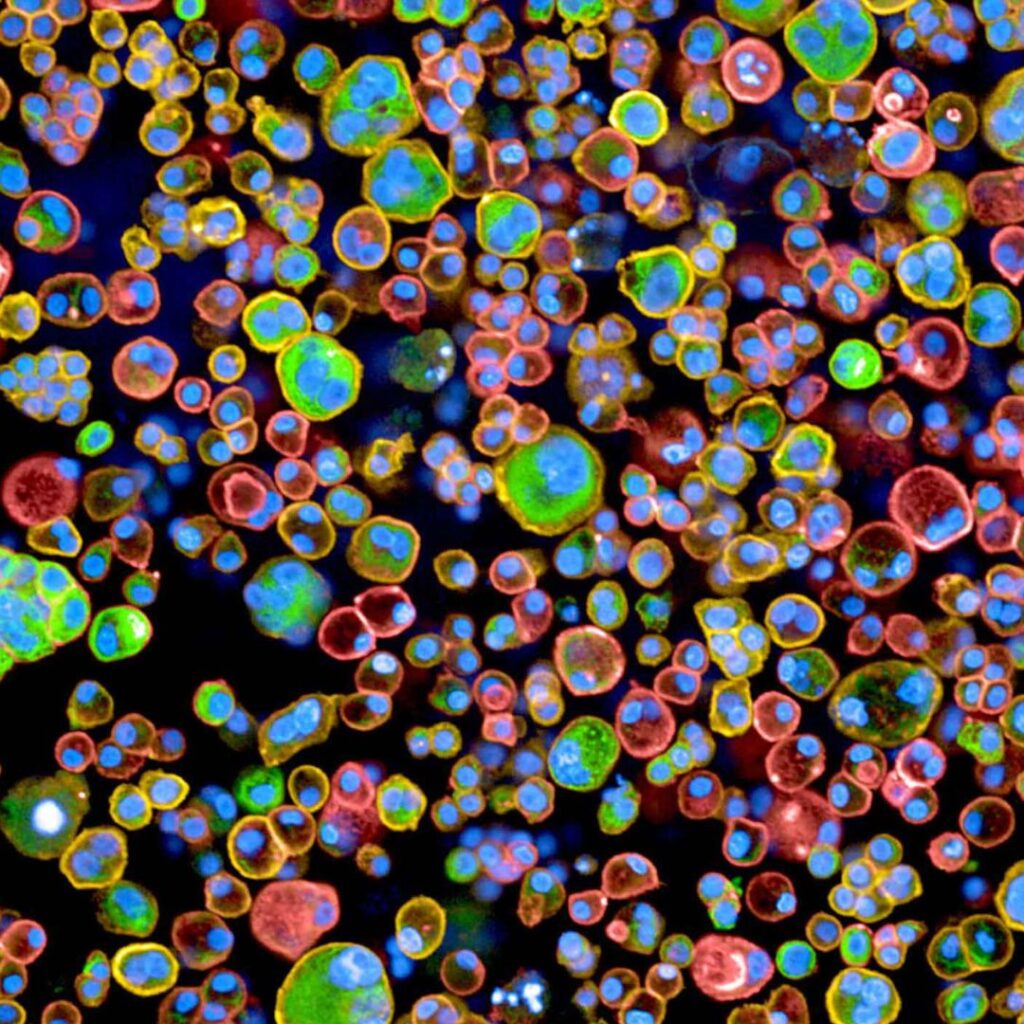
The evolution of cancer cell clones
Projects: Honours or PhD
Project details
Primary Supervisor: Associate Professor Guy Lyons
Supervisory Team: Guy Lyons, Mojdeh Abbasi
Centre: Cancer Innovations
Cancers are causes by mutations in key regulatory genes that promote tumour growth and dissemination. Most tumours are multiclonal, being comprised of cells that have different mutations from other cells within the tumour. It is known that a high level of this genetic heterogeneity predicts poor patient outcomes, but the reason is not known. One possible reason is that different clones within a tumour have complementary mutations that enable them to behave more malignantly when they are together than when they are present as individual clones. This project investigates the role of symbiotic interactions between clones of cells in driving tumour progression. It uses live cell microscopy, molecular analyses and gene editing to identify what types of genes can interact in different individual cells. Computer simulations are used to predict the effects of these cell-cell interactions on the population of cells as a whole, and how they affect the clonal evolution of the cells.
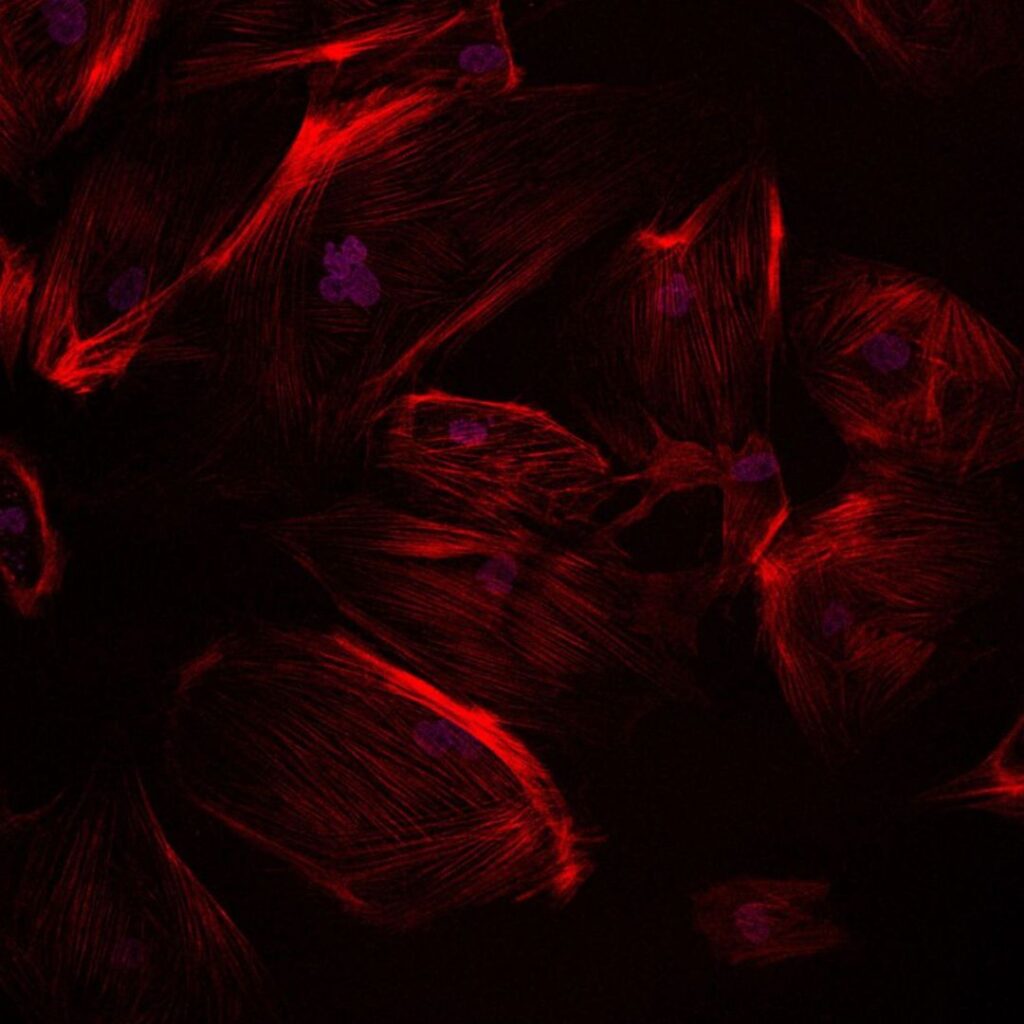
Identifying Circulating Tumour Cells through patient liquid biopsies
Projects: Honours, Masters & PhD
Project details
Primary Supervisor: Dr Dannel Yeo
Supervisory Team: Anna Leach, Christine Lee
Centre: Cancer Innovations
Our laboratory aims to improve low surviving cancers (pancreatic cancer, small cell lung cancer, mesothelioma, peritoneal, appendiceal, and colorectal cancer) through a personalised approach using liquid biopsy (circulating tumour cells) and patient-derived organoids (3D culture models). We utilize next generation liquid biopsy technology to detect and isolate rare cancer cells in the blood as a diagnostic and prognostic biomarker. Through single-cell characterisation, we can obtain molecular insights in a non-invasive manner. We also explore novel therapies such as targeted therapy and CAR-T cellular immunotherapy to target cancer vulnerabilities and obtain cures. We work closely with our clinical collaborators at Royal Prince Alfred Hospital and Chris O’Brien Lifehouse to ensure our findings have the best possible outcomes for cancer patients. Our translational research projects can be tailored to suit Honours, Masters or PhD degrees
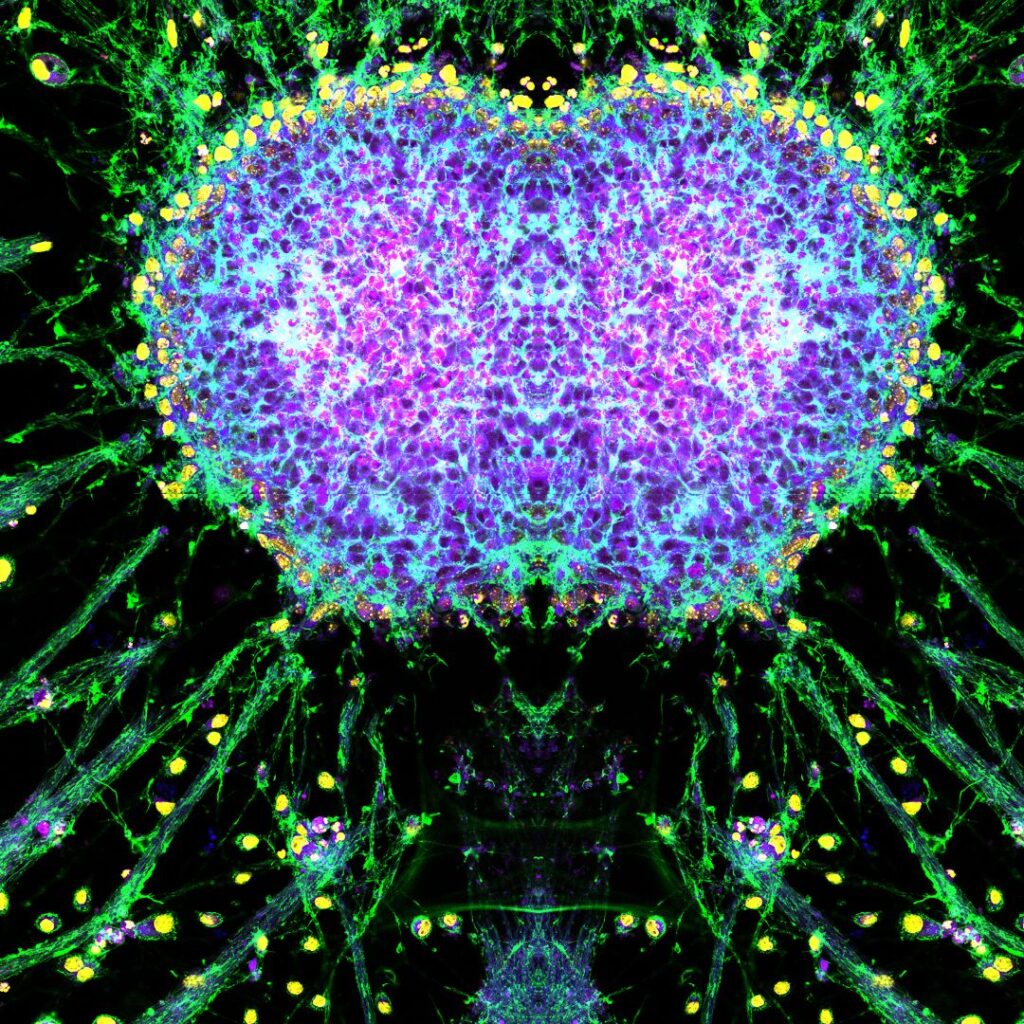
Investigating proteases in chronic liver disease and hepatocellular carcinoma
Projects: Honours
Project details
Primary Supervisor: Dr. Bobby Boumelhem
Supervisory Team: Professor Mark Gorrell; Dr. Jiali Carrie Huang
Centre: Cancer Innovations
Primary liver cancer is the 5th leading cause of cancer related deaths in Australia with incidence rates increasing yearly. The pathogenesis of chronic liver injury and cancer is driven by chronic cell death, proliferation and inflammation. Proteases are enzymes that cleave peptide bonds within proteins, often with regulatory outcomes in physiological and pathological processes. Proteases can regulate the structure, localization and function of many proteins, and influence protein-protein or protein-cell interaction crucial in disease pathogenesis, including cirrhosis and cancer. As such, our lab is keenly interested in the dipeptidyl peptidase (DPP) family of enzymes in chronic liver disease including cirrhosis and hepatocellular carcinoma. Fibroblast activation protein alpha (FAP), a member of the DPP family, is a unique protease with increase abundance in abnormal human tissue, especially in tissue-remodelling that occurs in injury, fibrosis and tumours. A project will be derived based on student’s interests in chronic liver disease and/or liver cancer. We are equipped with multiple mouse models of chronic liver disease including liver cancer as well as treatment with exciting and novel pan-DPP inhibitors.
Mechanisms of epithelial stratification
Projects: Honours or PhD
Project details
Primary Supervisor: Associate Professor Guy Lyons
Supervisory Team: Guy Lyons, Mojdeh Abbasi
Centre: Cancer Innovations
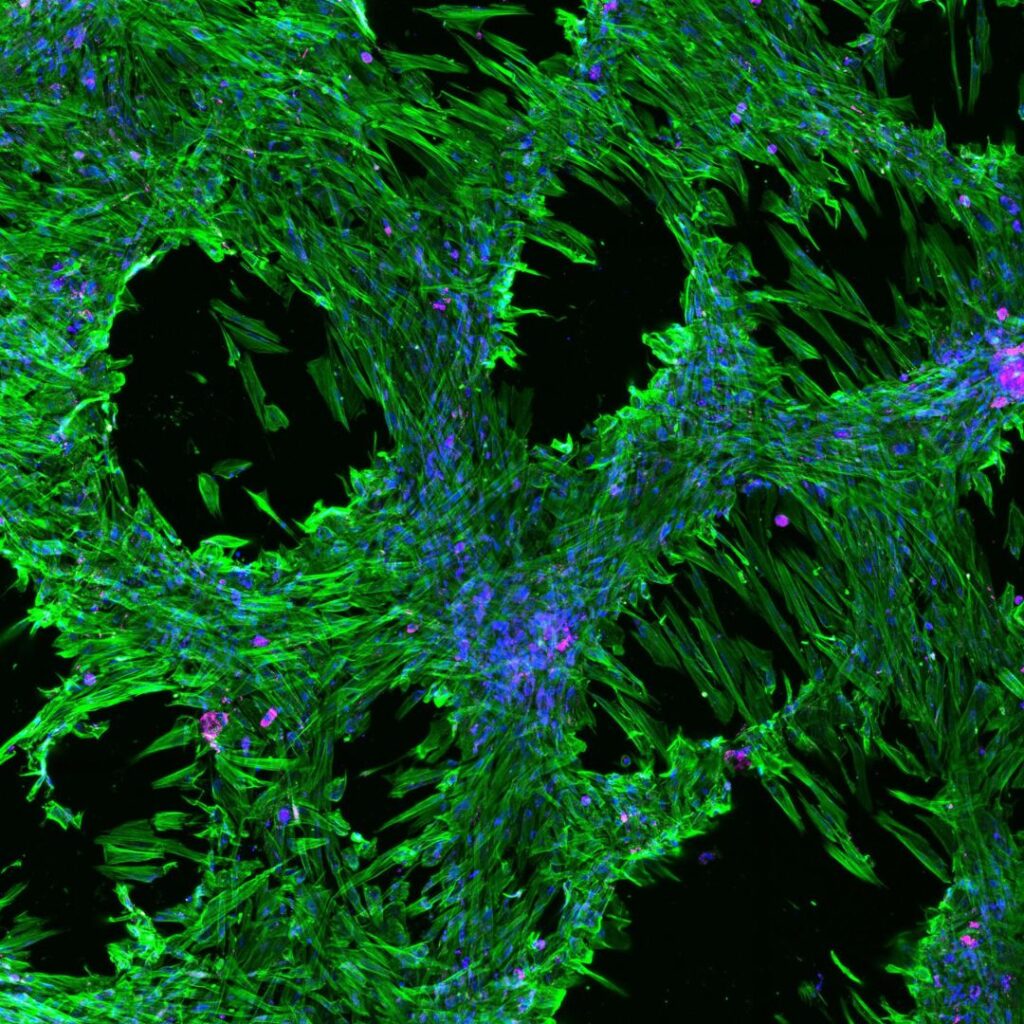
The epithelial cells that cover the surfaces of our skin, corneas and oral mucosa are multilayered, or “stratified”. This provides physical strength to resist abrasion and forms a barrier to the movement of molecules, microorganisms and UV radiation. In contrast, the “simple” epithelial cells that line the intestines, lungs and glandular tissues grow as a single, 2-dimensional layer. This simple growth pattern is relatively fragile, but facilitates the rapid passage of molecules across it. Thus, the ability to grow as a 3-dimensional array of cells is the characteristic that defines the distinction between these two fundamental types of epithelia, but the cellular mechanisms that regulate stratification are poorly understood. Mutations in the genes that regulate epithelial stratification could conceivably contribute to epithelial cancers by enabling inappropriate stratification without the blocks to cell replication that normally accompany it. In this project, the student will investigate epithelial stratification using a human corneal epithelial cell line grown in culture. The roles of particular genes in epithelial stratification will be determined by altering their expression using gene editing and/or RNA interference approaches. The degree of stratification and organisation of the cells will be determined from live cell imaging and immunofluorescent staining combined with advanced laser-based microscopy techniques.

Identifying Circulating Tumour Cells through patient liquid biopsies
Projects: Honours, Masters & PhD
Project details
Primary Supervisor: Dr Dannel Yeo
Supervisory Team: Anna Leach, Christine Lee
Centre: Cancer Innovations
Our laboratory aims to improve low surviving cancers (pancreatic cancer, small cell lung cancer, mesothelioma, peritoneal, appendiceal, and colorectal cancer) through a personalised approach using liquid biopsy (circulating tumour cells) and patient-derived organoids (3D culture models). We utilize next generation liquid biopsy technology to detect and isolate rare cancer cells in the blood as a diagnostic and prognostic biomarker. Through single-cell characterisation, we can obtain molecular insights in a non-invasive manner. We also explore novel therapies such as targeted therapy and CAR-T cellular immunotherapy to target cancer vulnerabilities and obtain cures. We work closely with our clinical collaborators at Royal Prince Alfred Hospital and Chris O’Brien Lifehouse to ensure our findings have the best possible outcomes for cancer patients. Our translational research projects can be tailored to suit Honours, Masters or PhD degrees
The role of sex chromosomes in melanoma survival
Projects: Honours, Masters & PhD
Project details
Primary Supervisor: Dr Jessamy Tiffen
Supervisory Team: Dr Cindy Tseng
Centre: Cancer Innovations
Men are more than twice as likely to die from melanoma compared to women, and our research aims to uncover why. We propose that genes located on the sex chromosomes may play a critical role in shaping the body’s ability to combat cancer, potentially explaining the survival advantage seen in women. Our team has identified several X and Y chromosome-linked genes implicated in anti-tumour responses, but the mechanisms behind their protective effects remain unclear. Using cutting-edge technologies such as CRISPR and Genetically Engineered Mouse Models, we are investigating how these genes function in both melanoma and immune cells through advanced pre-clinical models. Students joining this project will gain hands-on experience in cell and molecular biology, working with sophisticated in vitro and in vivo melanoma systems. Collaborating closely with clinicians from Melanoma Institute Australia, our research is designed to have real-world impact and translational relevance. Projects can be tailored to suit Honours, Masters, or PhD degrees, offering a unique opportunity to contribute to life-saving cancer research
Get in touch
To get in touch and for all general enquiries relating to our work, please contact Dr. Jessamy Tiffen.







